Health Equity and Telehealth
By Raymond Lowe, SVP/ CIO, AltaMed Health Services
Before 2020 there had been forward-thinking discussions on the consumerism of medicine, but the pandemic forced providers to focus on patient-centric care through telehealth, chatbots, remote consults, remote patient monitoring, and rich digital engagement tools. Fortunately, all stratifications of health care (payer, Medicare, and Medicaid) have benefited from this transformation. Some health systems saw up to 80% of ambulatory visits delivered by telephonic / telehealth encounters, but how do we ensure that all community members receive the care they need?
According to the Centers for Disease Control (CDC), health equity is achieved when every person has the opportunity to “attain his or her full health potential,” and no one is “disadvantaged from achieving this potential because of social position or other socially determined circumstances.” Health inequities are reflected in differences in length of life, quality of life, disease rates, disability, death, the severity of disease, and access to treatment. Telehealth can improve health outcomes, reduce reliance on emergency room visits for episodic care, and reduce hospitalizations – all of which help meet health care’s quadruple aim – reduce cost, improve patient experience, improve quality and physician joy of practice.
To determine how vulnerable a community is, we employ the Center for Disease Control (CDC) / Agency for Toxic Substance and Disease Registry (ATSDR), Social Vulnerability Index (CDC/ATSDR/SVI) tool that uses census data to determine the social vulnerability of every census tract. At AltaMed, by leveraging the CDC/ATSDR/SVI for social determinants of health (SDOH), we service and focus on the communities in the most vulnerable quartiles and overlay the SVI census track, and then geo-target by quartile of vulnerability. In April 2020, AltaMed Health Services started offering HIPAA compliant telehealth visits and they were not integrated with the Epic EMR. Today, we have full integration that allows the clinician to view the patient during the visit and invite in a translation service if needed. The incorporation of language services reduces language barriers is a key step toward health equity.
From May through December 2020, over 80,000 telehealth visits were completed. When it came time to vaccinate our patients, we used text messaging, email, and phone campaigns that leveraged the demographic data within our EMR to prioritize delivery aligned to CDC tier definitions. Furthermore, we broadly opened our vaccination slots to the community, so that everyone who wanted a COVID-19 vaccine could get one.
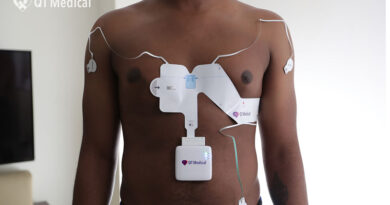
As we approach the midpoint of 2021, we look to broaden and continue extending our tele-footprint, including remote patient monitoring for Congestive Heart Failure (CHF). We enrolled a cohort of patients in January and have had promising results. We provide the patients with Bluetooth-enabled devices (weight scale, pulse oximeter, and BP cuff) and are taking daily measurements that are transmitted back to our virtual care team, where we can monitor changes in the patient and have a clinician intervene early. Daily rolling measurements are tracked and alerts are provided to the care team, enabling them to intervene versus having the patient go to the emergency room. Soon, we will be expanding this for Chronic obstructive pulmonary disease (COPD) and maternal-child/postpartum support for women.
Looking ahead from a care delivery perspective, with telehealth, we should have improved workflow, adoptions, and the technology should be easier to use for both providers and patients.
Looking ahead from a care delivery perspective, with telehealth, we should have improved workflow, adoptions, and the technology should be easier to use for both providers and patients. Primary care will see video specialty care, broader adoption for behavioral health, and routine care/nurse visits will become more prevalent. Quality outcomes will improve with advancements in remote patient monitoring that focus on the patient-centric home for those with chronic conditions.
We need to be careful that we do not revert to all our traditional care delivery models, maintain the focus to continue to strive and deliver patient-centric care that is consistent for all patients, and not lose the valuable legacy of learning from the pandemic.
Key Findings and Implications for the Future
- Telehealth must be patient-centric, intuitive, and as simple as clicking a link.
- Insignificant broadband coverage can result in the patient defaulting to telephonic visits versus full video. We need to eliminate the digital desert that exists in socially disadvantaged communities that include urban cities and rural communities. Fortunately, there are national and state bills pending legislation review: 1) Life America Act for Health Infrastructure and 2) Broadband and Investments in America’s Health Infrastructure.
Providers should have the ability to work from anywhere and launch the tele encounter from a mobile device or laptop. Exam rooms may need to be altered to optimize telehealth visits and creation of telehealth centers of excellence is recommended.