M-health modeling implementation and operation
By Dr. R. A. Ramanujuan, MD Physician, Diabetic Care Associates, and
Dr. Anu Banerjee, PhD, MS MHM, Chief Quality and Innovation Officer, Arnot Health
M-health is a platform for the rapid exchange of abundant information about patient medical records. Accomplishing desirable health-related service should guarantee technological support for robust bidirectional transaction between patients and providers. It is often, distinctive to illness to espouse acceptance with perceptible value to stakeholders with information that is reliable to engage with commitment and confidence. Germane medical conditions where such streaming data conceptually, is attractive are those where numerical data extraction is critical to outcome; such as hypertension, diabetes and many of the cardio-metabolic disorders “Facilitative patient relay”. In the management of hypertension, diabetes, obesity and other cardio metabolic disorders, live stream facilitative patient-clinical care giver interaction is critical. Patient’s can securely access clinical information; such as blood sugar, blood pressure, weight, exercise, and cholesterol, through affordable devices. The process of data generation on health risk determinants directly from customers or by outsourcing through allied health care givers, allow better understanding of information collected at informal sites. It is possible to access and fuse this raw data from diverse locations at secure sites for validation, integration and dissemination. Today’s Healthcare is assembled on a single, formal platform to react to signals generated during clinic visits and globally, the stream in clinic workflow is structured to react to medical issues associated with the subjective component and much less for those without any symptoms as with early cardiometabolic changes. Major cardiometabolic disorder-related complications are due to deficiencies in the integration of emerging changes in silent risk factors such as blood pressure, blood cholesterol, blood sugar, weight, smoking, race and gender and many more. Consequently, detection and clinical reaction in these conditions are delayed until there is significant biological damage to vital organs. Coronary heart diseases, stroke, chronic kidney disease, peripheral vascular diseases due to diabetes, cholesterol and hypertension are complications due to time-dependent cumulative changes.
We believe that m-health will allow under-served populations from all locations to engage with caregivers’ for synchronized clinical care.
Technology and analytics can integrate datasets as panels and detect the beginning of the rise in risk by sequenced segments to support early detection through device system behavior. Factors like obesity, smoking, high blood pressure, diabetes, high cholesterol, exercise, gender, race, smoking, alcohol ingestion and socioeconomic stratum alone or in combination is a significant economic and health burden. The operation implementing risk-adjusted flow of information is similar to the preventive approach in the management of communicable diseases such as Tuberculosis and HIV. Novel system behavior and analytical options can support similar preventive health care strategy in cardiometabolic disorders. In the future, it will be possible to integrate structured exercise performance measures through advanced system behavior. In the technology arena, data access through affordable device, modifiable system behavior and analytical process hold promise to support primordial clinical care in cardiometabolic disorders. The development of supportive panels on relevant clinical data sets is important in the management of cardiometabolic disorders. There should be plans to support preemptive action plan in the management of cardio metabolic disorders. Appropriate response measure is the integration of therapeutic lifestyle changes such as diet and exercise. As we are aware, current electronic medical records known as EMRs are not equipped to support easily identifiable comprehensive and condition-specific linear data collection on risks. The process of implementation and execution of operation will be a creative revolt that extent clinical care beholds. It will be essential to reframe data acquisition sites from clinics to unfamiliar resource access instruments to develop this cultural change within the healthcare system. The accommodation of allied health forces and reforming external service integration will be a challenge and a cultural shift from office-based practice that providers are bound to practice today in healthcare. There is a huge data deficiency in integration between healthcare vendors and no standard formats exist today. Blood pressure, pulse and blood sugar values are not steady physiological values yet, decisions are based on observations made in confined clinical locations. This operation is incapable to reconcile ecological and contextual perturbations. Implementation of m-health based operation has become reality in practice and wider acceptance holds promise to the economic model of collaborative service with public health and clinic-based service.
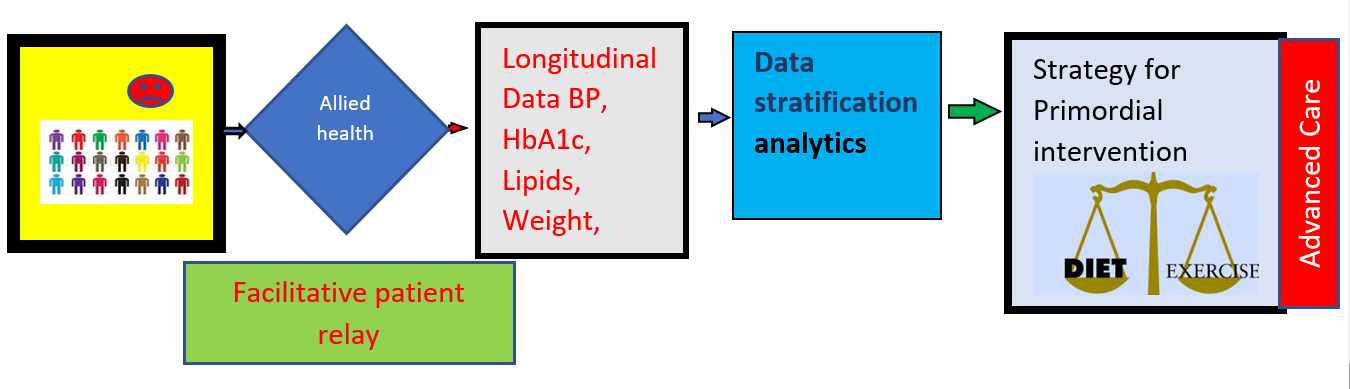
Summary: We believe the future m-health operational systems can behave as a proxy to electronic health records and curate biological risk factors and set the standard for integration of condition-specific complex Marko’s mathematical algorithms through bioinformatics for mapping early detection and intervention both at individual and population level.
We believe that m-health will allow under-served populations from all locations to engage with caregivers’ for synchronized clinical care. The proposed facilitative patient relay operation represents prudent participatory patient-centered efficacious intervention. M-health visits can reduce office visits and permit continuous vigilant interaction between patients and providers in chronic disease conditions.



